Over the last decade, three of the most ordinary drinks in the American kitchen — drinks most of us pour without a second thought — have been quietly accumulating a paper trail in some of the world’s most respected medical journals. Individually, each one looks harmless. Together, and consumed the way most adults actually consume them, researchers at Oxford, Harvard and the Mayo Clinic have begun documenting a measurable effect on the parts of the brain responsible for memory, focus and emotional regulation.
None of this is front-page news. There has been no surgeon-general press conference, no product recall, no dramatic headline. Just a slow, careful accumulation of peer-reviewed evidence — and a growing group of physicians, neuroscientists and dietitians who have begun, quietly, to change their own habits.
The short list, in plain language
The three drinks now being flagged by clinicians are not exotic. You almost certainly have at least one of them in your refrigerator right now.
- High-caffeine energy drinks (and large afternoon coffees). Not caffeine itself — which, in moderation, is among the better-studied cognitive enhancers we have — but the specific pattern of consuming 160–300 mg of caffeine in the afternoon, on top of chronic stress and poor sleep. Lab studies have repeatedly shown this pattern elevates cortisol, the body’s primary stress hormone, and in habitual users it keeps the stress response running a little hotter than it should [1][2].
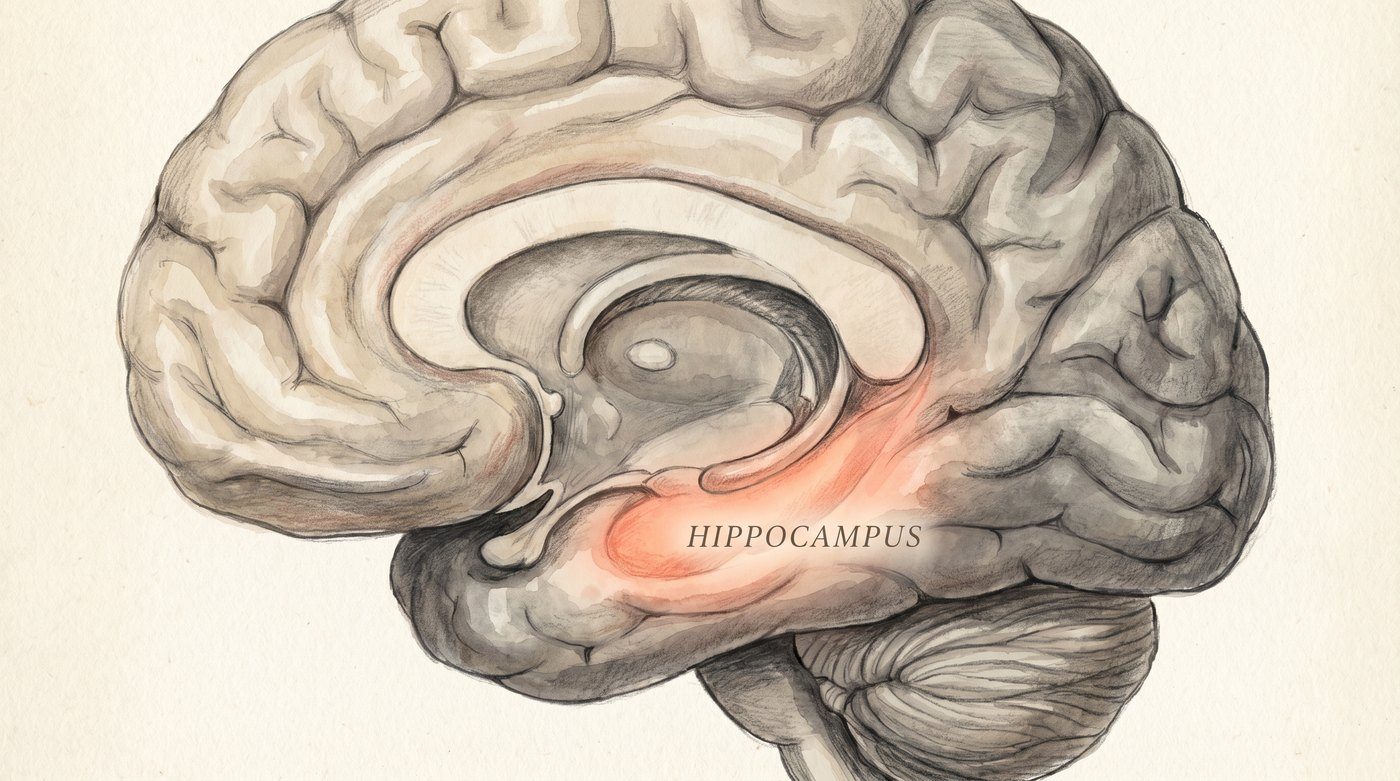
- The “harmless” evening nightcap. A single glass of wine, a small whiskey, a beer before bed. A 30-year longitudinal study published in The BMJ followed 550 adults, imaged their brains, and found that even moderate alcohol consumption was associated with a higher risk of hippocampal atrophy — the hippocampus being the brain region responsible for forming new memories [3]. Alcohol also specifically disrupts REM sleep, the stage most tied to memory consolidation [4].
- Ultra-sweetened sodas (regular and, surprisingly, diet). In a large Framingham Heart Study cohort published in Stroke, higher consumption of artificially-sweetened diet soda was associated with a higher risk of stroke and memory loss over ten years of follow-up [5]. Regular sugar-sweetened sodas have been independently associated with smaller total brain volume and poorer episodic memory performance [6]. Again: association, not proof of causation — but a pattern researchers no longer describe as trivial.
Why your brain notices these three drinks in particular
Your brain runs on a remarkably narrow set of conditions. It needs steady glucose, steady oxygen, steady sleep, and — the part most of us forget — steady time with the stress response turned off. Each of the three drinks on the list above quietly undermines one of those conditions. Afternoon caffeine leaves the stress response on long after we want it off. The evening nightcap blocks the sleep stage our brain uses to consolidate the day. Ultra-sweetened sodas spike the vascular system the brain depends on for every calorie of thinking.
And here is the part almost nobody tells you. The brain does most of its actual repair work between 11 p.m. and 5 a.m., during deep sleep and REM. If you have spent the previous twelve hours in a mildly elevated stress state — and then capped it with something that disrupts sleep architecture — you are asking the nervous system to do its hardest job under its worst conditions. For most of us, for most of our lives, that has been the unspoken deal. Researchers are starting to ask whether the deal is as harmless as we assumed.
Nightwell angle: the second drink on the list is the one almost nobody examines
On a Sunday night last February, a 58-year-old retired teacher named Maureen sat at her kitchen counter with the same small glass of merlot she had poured almost every night for fourteen years. “It’s not the wine that worries me,” she told her daughter on the phone. “It’s that I opened the fridge this morning and genuinely could not remember why.”
Maureen is not a heavy drinker. She is, by every reasonable measure, a "moderate" one: somewhere between seven and ten standard drinks per week, most of them on her sofa, most of them before bed. Her annual physicals come back clean. Her doctor has never expressed concern. And yet — a growing body of careful, longitudinal, peer-reviewed research says she should probably be asking better questions.
The problem is not the wine. The problem is what your brain tries to do between 2 and 5 in the morning — and why a drink before bed prevents it from finishing.
What the Oxford data show
In 2017, a team at Oxford published a 30-year longitudinal study in The BMJ. They followed 550 adults, imaged their brains, and tested memory and decision-making throughout. The finding that made headlines — and was then very politely buried in dinner-party conversations — was this: even moderate alcohol consumption was associated with a higher risk of hippocampal atrophy. The heavier the drinking, the more atrophy. But the dose-response curve did not bend down to zero at "just a glass or two." It bent down somewhere closer to none [3].
What actually happens to the sleeping brain
Sleep is not a single state. It is a carefully choreographed procession of stages that cycles through the night. Two of them matter most for cognition: slow-wave (deep) sleep, which clears metabolic waste, and REM sleep, which consolidates memory, regulates emotion, and solves the problems you couldn’t solve awake.
Alcohol famously helps people fall asleep — the subjective "calm" part of the nightcap effect. What it does in the next four to six hours, however, is something different. As the body metabolizes the alcohol it rebounds: REM is suppressed in the first half of the night and fragmented in the second. Wake episodes increase. Overall sleep architecture looks, on a lab polysomnograph, as if someone had driven a small truck through it [4]. And this is for "one or two drinks."

The characteristic signature of an alcohol-disrupted night: falling asleep easily, then waking between 2 and 4 a.m., heart racing, mind alert.
Why it matters after 50 — and honestly, before 50
In our late 40s and 50s, two things converge. Growth hormone — which drives physical recovery during slow-wave sleep — declines naturally. Estrogen (for women) and testosterone (for men) shift in ways that already make deep sleep harder to achieve. A nightly alcohol habit does not cause any of that. It simply keeps the brain from doing the repair work it has fewer hours available for in the first place.
The new evening ritual: same 10 minutes, different tool
The good news is that the neuroscience of the opposite ritual — actively down-regulating the nervous system before sleep — is unusually clean. A short, guided focused-attention practice in the twenty minutes before bed has been shown to shift EEG patterns toward slower, more organized rhythms and to make the transition into restorative sleep easier [7]. The challenge, as anyone who has tried, is that asking a tired adult to "meditate" without feedback is like asking her to hit a nail blindfolded.
A wearable that lets you hear your own brain calming down
The Muse 2 Brain Sensing Headband, made by InteraXon, uses seven medical-grade EEG sensors resting lightly on the forehead and behind the ears to detect the brain’s electrical patterns in real time. During a wind-down session, the headband translates those patterns into a soundscape: the calmer your mind, the calmer the weather you hear through your earbuds. When attention drifts — ruminating about a meeting, rehearsing tomorrow’s to-do list — the wind picks up. You don’t have to try to fix it. The brain corrects itself, because for the first time it can hear what it’s doing.

Ten minutes before bed: a slim headband, a short soundscape, and a brain that finally gets to rehearse the state it will spend the night in.
What the swap actually looks like — in calendar time
Most of the readers who wrote in after our March feature described the same evening routine. It looks like this:
- 9:40 p.m. Kitchen closed. No alcohol after this hour.
- 10:05 p.m. In bed, lamp on low. Muse 2 headband on. Phone in airplane mode.
- 10:08–10:18 p.m. A ten-minute guided wind-down through the Muse companion app.
- 10:20 p.m. Headband off, lamp off, done.
Ten minutes. That is the entire change. The readers who stuck with it described, within three weeks, shorter time to fall asleep, fewer 2 a.m. awakenings, and mornings that start at a different energy level. Nothing dramatic. Nothing miraculous. Just a brain that stopped being asked to repair itself through a chemical headwind.